Sunday, May 29, 2022
This Is Not How You Treat Frozen Shoulder
Sunday, May 22, 2022
Do Softer Running Shoes Cause More Injuries?
 |
| Vaporfly from Nike |
It will also affect how you perceive aches and pain received from running during the study. It will probably not be possible to tell whether it was the softer midsoles, heel drop, lightness or other differences that gave you grief.
To avoid this, researchers in this study collaborated with Decathlon to make custom running shoes that cannot be visually distinguished and only has one single technical detail different for each experiment. Both researcher and subject were not aware (double blind) which type of shoe was used.
I have written before that runners, new to wearing shoes with thicker midsoles, tend to land more heavily and with greater force. This is even after running with the shoe for more than 6 weeks. This has become what is known as the shoe cushioning paradox, where more cushioning leads to runners landing more heavily, with a lesser chance of getting injured.
Decathlon made 2 prototypes, each with an inch thick of midsole. Half the soles had soft cushioning while the other half had firmer midsoles, which were randomly assigned to 848 runners. These runners completed a treadmill test to assess stride characteristics and were then monitored for 6 months.
Stride analyses showed that runners land more heavily when wearing the shoes with the softer midsoles.This is similar to other studies, which may cause more injuries (not less).
However, the runners wearing the shoes with firmer midsoles were 52 percent more likely to get injured during the follow up period (perhaps to suggest injury protection offered by the softer cushioning). This is similar to the shoe cushioning paradox. How is this so?
What the researchers found was the timing of impact matters. When your foot strikes the ground, there are 2 distinct impacts. The first impact occurs when your lower leg slows down suddenly after striking the ground. The second impact which occurs a few milliseconds later is the larger force caused by the rest of your body. The first impact is the one researchers suspect is linked to injuries.
This force is greater in runners with the softer midsoles, but the softer midsoles slow down that first jolt and spreads it out over a longer period of time causing it to overlap with the second impact. This combined impact makes the total force appear greater thus giving the impression that softer midsoles cause runners to land harder.
After separating the first and second impacts into 2 differerent values, the authors found that the first impact (the one linked to injuries) was actually smaller with the softer midsoles.
Does this mean we should now run with shoes with the thickest and softest midsoles? Afterall, they do lighten the load on your joints and reduce injury risk. At least that's what the study by Malisoux et al (2022) suggest.
Do note that these Decathlon made shoes for the study are different from the ones available in stores. Morever, with each different brand, they have different technologies and use different materials.
Just like the newest generation of Vaporfly (with its super thick soles and carbon plate), it still remains questionable whether it reduces injury risk, with the carbon fiber plate(s) still untested.
The midsole thickness definitely makes your foot more unstable especially when going around sharp corners or while making a u-turn in an out and back route. Only time and another specifically designed study can tell us more.
Even the authors concede that very little is known about the complex links between running shoes and injuries. I do like their suggestions, that is to stick with whatever you're running with, if you are happy with them. If you do switch shoes, consider carefully why you're switching, do try several designs and take you time making the switch. Also consider alternating types of running shoes to vary the stress on your body.
Just like what I've been telling my patients.
Reference
Malisoux L, Gette P, Backes A et al (2022). Lower Impact Forces But Greater Burden For The Musculoskeletal System In Running Shoes With Greater Cushioning Stiffness. Eur J Sp Sci 19: 1-11. DOI: 1080/17461391.2021.2023655
Sunday, May 15, 2022
Need To Poop Mid Race?
 |
| Familiar sight at races |
How and why does this happen?
It all starts at the lining of our gut (or alimentary canal from the stomach to the anus, consisting of the small and large intestine), which has 2 jobs. First, it allows food to pass from the gut to our bloodstream and it also prevents nasty bacteria and toxins from entering the same route.
When we exercise, blood from our digestive organs (up to a quarter of our blood) are diverted to our muscles to supply more oxygen to them. Moderate exercise can reduce the blood supply to the gut by up to 70 percent.
During prolonged endurance exercise (usually longer than 2 hours at 60 percent VO2 max or more), the gut lining starts to malfunction since it is now lacking oxygen and energy. Food that the gut is trying to absorb gets blocked while toxins start to leak into our bloodstream.
In addition, the bouncing and jostling from exercise can cause direct mechanical damage to the lining of the gut. This is why GI issues happen more with running compared to cycling.
Heat and dehydration will divert more blood away from the gut, allowing more gases and/ or toxins to pass through.
What's worse with GI distress is, it often gets worse when you're anxious or stressed, for example before your big race. Anxiety and psychological stress trigger adrenaline which further diverts blood away from the digestive system while increasing leakage in the gut lining.
How do we prevent it? In a perfect world the obvious approach would be to find out the food that triggers our GI distress and avoid them prior to our races and long training sessions.
Studies show that a class of poorly digested carbohydrates known as FODMAPs (fermentable oliosaccharide, disaccharide, monosaccharides and polyols) may cause GI distress for many of us as they are not well absorbed in the small intestine. This causes fermentation and produce gas in the colon.
This include food containing wheat, milk, onions, garlic, legumes (beans, peas and lentils) and stone fruit (apricots, peaches, plums, mangoes, lychees etc).
Timing matters too, as eating too much fat, protein or fiber 90 minutes before exercise may increase the risk of GI problems.
Please note that people who keep to low FODMAP diets tend to have less healthy and diverse gut microbiomes.
Personally I've found that 'training your gut' works well. Many other athletes I've spoken to and treated say that eating and drinking energy gels/ bars and sports drinks that are palatable over time makes them less susceptible to GI issues.
You have to try them out during your long training sessions or less important races. A gel or bar may taste fine at room temperature, but may taste terrible and be difficult to swollow in hot, humid conditions. Research suggests that 2 weks of training the gut can make a difference (Miall et al, 2018).
All the best to Donaben and the rest of Team Singapore at the Hanoi SEA Games.
References
Miall A, Khoo A, Rauch C et al (2018). Two Weeks Of Repetitive Gut Challenge Reduce Exercise-associated Gastrointestinal Symptoms And Malabsorption. Scand J Med Sci Sports. 28: 630-640. DOI: 10.1111/sms.12912
Smith KA, Pugh JN, Duca FA et al (2021). Gastrointestinal Pathophysiology During Endurance Exercise: Endocrine, Microbiome And Nutritional Influences. Eur J Appl Physiol. 122(10): 2657-2674. DOI: 10.1007/s00421-021-04737-x
*I did not write about probiotics (supplements) as they are capable of producing a good environment in the gut but do not eliminate symptoms entirely. That's my personal experience as well. Plus 3 out 5 of this review's authors receive research funding from companies that make supplements.
Sunday, May 8, 2022
What Really Wears Out Your Joints
 |
| Picture by Dr Howard Luks |
I've written previously that running will not wear out your knees (or your joints). So what does? There is now evidence that OA is not due to a mechanical wear and tear process. Even if you already have OA, exercise will not wear out your joints quicker.
Of course there are mechanical causes of OA. People who are severely bow legged or have severely knocked knees can be more prone to developing OA since one side of the knee joint is over loaded. Certain fractures near a joint can lead to post traumatic OA (due to mal- alignment).
Patients whose meniscus is torn and subsequently removed have an increased risk of developing OA. Which is why surgeons now rarely remove the whole meniscus, just the torn bit.
So, what causes arthritis in our joints? For those without any previous injuries to the joint, we have hundreds of proteins, cytokines, chemicals and other compounds that forms the articular cartilage, which lines our joints. When the joints are in good health, these chemicals support articular cartilage health and nutrition.
We do not know exactly why, whether it is due to injury, our diet, metabolism or weight that, OA develops. It may be all of the above when a 'switch' flips. Changes in the joint(s) similar to changes associated with other chronic diseases happens. That switch causes an increase the production of chemicals that harms our articular cartilage (Wang et al, 2015).
Over time, these chemicals cause injury to the articular cartilage cells. This weakens the articular cartilage and its ability to withstand load and stress.
The articular cartilage can become thinner when not functioning well. This can lead to inflammation, swelling, warmth and pain. This chronic low grade inflammation is what appears to cause OA. This is the same chronic inflammation thought to cause other chronic diseases like heart disease, fatty liver and Type II diabetes.
Researchers are still trying to understand how all these proteins and substances affect articular cartilage health and the incidences of OA.
Exercise has actually been proven to decrease the concentration of these proteins and substances that harm our articular cartilage.
Helmark et al (2010) showed that IL-10, a chemical that protects articular cartilage in the knee was produced in response to exercise. Similarly, COMP (a protein that is a marker of cartilage degeneration) was decreased in the knee with exercise.
Another research paper by Hyldahl et al (2016) demonstrated that running was associated with a decrease in cytokines (chemicals) in the knee related to articular cartilage wear and tear.
Studies are suggesting that metabolic health definitely plays a bigger role in causing OA. Yes, other than Type II diabetes, dementia, high blood pressure and heart disease, metabolic issues are also thought to be involved in the development of OA. All tissues in our body, including our articular cartilage are sensitive to our dietary intake. The earlier we realize this, the better off we will be.
Too many health care professionals ask their patients to stop running (or exercise) to 'save' their joints. In actual fact, running and other knee exercises have been shown to relieve mild knee arthritis and does not harm articular cartilage.
Exercise has been unequivocally proven to be the most effective treatment for early and moderate OA in our joints. You do not have to stop exercising.
Let your symptoms be your guide. If there is no swelling and no pain, you can still run or exercise. Be careful with the distance, intensity and frequency of exercise. You may also want to cycle or swim occasionally. Or try a different shoe, or different running surface and/ or include a weight training session to get yourself stronger.
References
Helmark IC, Mikkelsen UR, Borglum J et al (2010). Exercise Increases Interleukin-10 Levels Both Intraarticularly And Peri-synovially In patients With Knee Osteoarthritis: A Randomized Controlled Trial. Arthritis Res Ther. 12, R126. DOI: 10.1186/ar3064
Hyldahl RD, Evans A, Kwon S et al (2016). Running Decreases Knee Intra-articular Cytokine And Cartilage Oligomeric Matrix Concentrations: A Pilot Study. Eur J Appl Physiol. 116 2305-2314. DOI: 10.1007/s00421-016-3474-z
Wang X, Hunter J and Xu CD (2015). Metabolic Triggered Inflammation In Osteoarthritis. OA and Cartilage. 23(1): 22-30. DOI: 10.1016/j.joca.2014.10.002
Sunday, May 1, 2022
Quads And Squats
I came across an interesting article summarizing the evidence of the relationship between muscle forces acting on the ACL. This is important since muscles around the knee can increase and decrease the strain and mechanical loads on the ACL. This presents opportunities for preventive intenventions.
Subsequently, our staff had interesting discussions regarding that article (referenced at the end of this post). The article demonstrated the forces acting on the knee joint and what can cause injuries there, specifically, what can hurt the ACL.
The article reviewed muscle and and ACL loads during knee bending as well as weight bearing tasks like walking, lunging, landing, jumping and sidestep cutting.
Ready for the results? The quadriceps (thigh muscles) and gastrocnemius (calf muscles) increases load on the ACL due to anterior shearing forces at the tibial (shin bone). This is especially so when the knee is straightened.
The hamstrings and soleus (deeper calf muscles) helps to unload the ACL by generating posterior tibial shearing forces. For the hamstrings to 'protect' your ACL, your knee has to be bent at least 20 to 30 degrees.
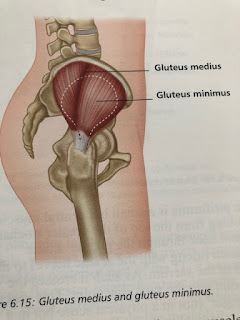 |
| R gluteus medius |
Surprised?
Patients who have been been told to strengthen their quadriceps (especially after ACL reconstruction) were really surprised when we told them. Make sure you focus on your hamstrings and soleus muscles instead.
The muscle to rule them all is of course the gluteus medius. Our patients will now understand why we always ensure their gluteus medius muscle is strong to prevent knee pain, Achilles tendon and of course ACL injuries.
Now you know.
Reference
Maniar N, Cole MH, Bryant AL et al (2022). Muscle Force Contributions To Anterior Cruciate Ligament Loading Sports Med. DOI: 10.1007/s40279-022-016743


.jpg)




